Most Common Sports Injuries: Types, Causes and Treatment
Information reviewed by: Dr Foo Gen Lin | Last updated:
Dealing with a sports injury that's keeping you from staying active? Dr Foo provides thorough assessment and personalised treatment to help you recover and return to the activities you enjoy.
MBBS (University of London) | MMed (Ortho) | FRCSEd (Ortho) | FAMS (Ortho)

What Are Sports Injuries?
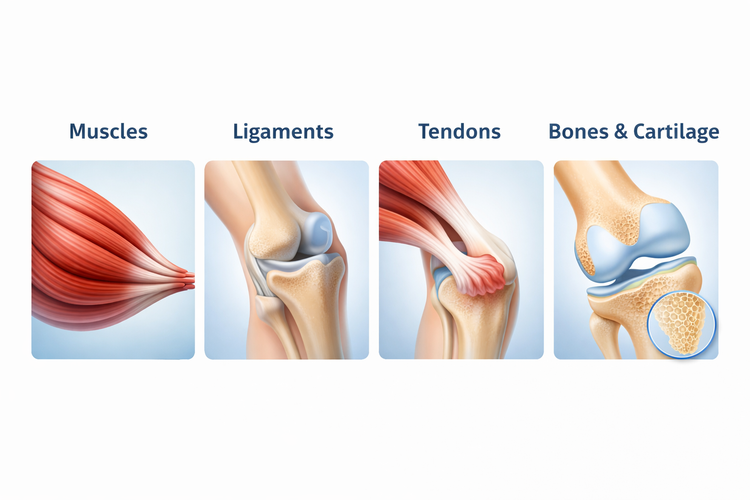
Sports injuries are physical injuries that occur during exercise or sporting activities,
affecting structures such as muscles, ligaments, tendons, bones, and
cartilage. They range from minor strains that resolve with rest to more severe
damage that may require surgery.
These injuries can affect anyone who is physically active, from recreational gym-goers to
competitive athletes. Some develop suddenly from a single incident, while others build up
gradually through repetitive stress on the body.
Understanding the most common sports injuries, their causes, and how they are managed can
help you recognise symptoms early and seek appropriate care.
What Causes Sports Injuries?
Sports injuries typically result from a combination of physical, environmental, and
training-related factors rather than a single cause. These are broadly grouped into two
categories.
Acute injuries happen suddenly during activity. A wrong landing, a direct
collision, or a sudden twist can damage ligaments, muscles, or bones in an instant. These injuries
are common in contact sports and activities involving jumping or rapid direction changes.
Overuse injuries develop gradually when repetitive stress is placed on a body part
without enough time for recovery. Tendons, bones, and muscles can break down faster than they
repair, resulting in conditions such as tendinopathy, stress fractures, and shin splints.
Several factors increase the likelihood of both types:
- Training errors, including rapid increases in intensity, volume, or frequency
- Previous injury that was not fully rehabilitated, which weakens the affected area and alters movement patterns
- Muscle imbalances or weakness, particularly around the knees, hips, and shoulders
- Insufficient warm-up before activity, which leaves muscles and joints less prepared for sudden demands
- Inadequate rest and recovery between training sessions
- Poor technique in movements such as landing, lifting, or throwing
- Inappropriate footwear or equipment for the activity
10 Most Common Sports Injuries
The following injuries account for the majority of sports-related conditions seen in orthopaedic and sports medicine practice. They are grouped by the type of structure affected.

1. Ankle Sprains
What it is: A sprain occurs when the ligaments supporting the ankle are
stretched or torn, most commonly on the outer side. The anterior talofibular ligament
(ATFL), which connects the ankle bone to the fibula (the smaller bone of the lower leg) and
prevents the foot from sliding forward, is the most frequently injured.
Ankle sprains account for an estimated 20 to 40 per cent of
all athletic injuries, making them the single
most common sports injury worldwide.
Cause: Rolling or twisting the ankle inward during landing, sudden direction
changes, or stepping on an uneven surface.
Frequently seen in: Basketball, football, netball, running, and tennis.
Common symptoms: Pain on the outer ankle, swelling, bruising, and difficulty
bearing weight. Severe sprains may produce a popping sensation at the time of injury. In some cases,
a severe twist can also result in an ankle
fracture, which requires imaging to rule out.
Some people develop chronic ankle instability if
sprains are not properly rehabilitated.
2. ACL Tears
What it is: A tear of the anterior
cruciate ligament (ACL), one of four major ligaments stabilising the knee. The ACL prevents
the shinbone from sliding forward and controls rotational movement.
ACL tears occur at a rate of around 69 per 100,000
people per year across studied populations, including the United States, Sweden, Iceland,
and Australia.
Cause: Sudden deceleration, pivoting on a planted foot, or landing awkwardly from a
jump. Most ACL tears occur without direct contact to the knee.
Frequently seen in: Football, basketball, skiing,
netball, and martial arts.
Common symptoms: A "popping" sound or sensation at the time of injury, rapid
swelling within hours, knee instability or a feeling of the knee "giving way," and difficulty
bearing weight.
3. Meniscus Tears
What it is: A tear of the meniscus,
a C-shaped piece of cartilage that acts as a shock absorber between the thighbone and shinbone. Each
knee has two menisci (medial on the inner side and lateral on the outer side) that help distribute
weight and cushion the joint.
Meniscus tears affect an estimated 12 per cent of
adults and can occur in those younger than 40 following acute trauma.
Cause: Twisting or rotating the knee while bearing weight, especially with the foot
planted. Degenerative tears can also occur over time with wear and repetitive loading.
Frequently seen in: Football, rugby, basketball, and running. More common in
athletes over 30 years old due to natural cartilage wear.
Common symptoms: Knee pain along the joint line, swelling that develops over 1 to 2
days, stiffness, locking or catching sensations, and difficulty fully straightening the knee.
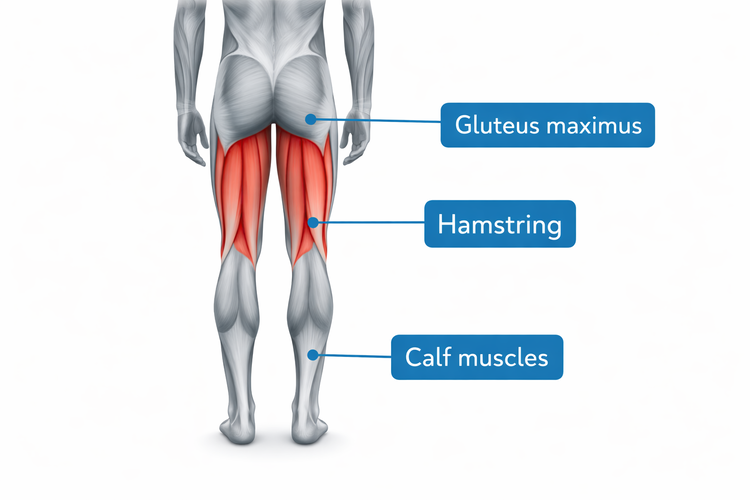
4. Hamstring Strains
What it is: A hamstring strain is a partial or complete tear of one or more
of the three muscles running along the back of the thigh. These muscles control knee bending
and hip extension.
Hamstring strains represent around 10 per
cent of all injuries in field-based team sports, and in men's professional football
they now account for up to 24 per cent of all reported injuries.
Cause: Overstretching the hamstring during sprinting, kicking, or sudden
acceleration. Muscle fatigue, poor flexibility, and inadequate warm-up increase risk.
Frequently seen in: Sprinting, football, rugby, and sports involving explosive leg
movements.
Common symptoms: Sharp pain at the back of the thigh, often during a sprint or
kick. Bruising, swelling, and weakness in the affected leg may follow. Severe strains may make
walking difficult.
5. Rotator Cuff Injuries
What it is: Damage to the rotator
cuff, a group of four muscles and tendons that stabilise the shoulder joint and allow
overhead arm movement.
Cause: Repetitive overhead motions (throwing, swimming strokes), direct impact to
the shoulder, or a fall onto an outstretched hand. Gradual wear over time can also weaken the
tendons.
Frequently seen in: Swimming, tennis, badminton, cricket, volleyball, and weight
training.
Common symptoms: A dull ache deep in the shoulder, pain when lifting the arm or
reaching overhead, weakness in the shoulder, and difficulty sleeping on the affected side.
6. Shoulder Dislocations
What it is: A shoulder
dislocation occurs when the upper arm bone (humerus) is forced out of the shoulder socket.
The shoulder is the body's most mobile joint, which also makes it the most prone to dislocation.
Global data estimates up to 56 shoulder dislocations per
100,000 people per year, with more than half of all cases being sports-related.
Cause: A forceful blow to the shoulder, falling onto an outstretched hand, or
extreme rotation of the arm during a tackle or collision.
Frequently seen in: Rugby, football, martial arts, basketball, and contact sports.
Common symptoms: Visible deformity of the shoulder, intense pain, inability to move
the arm, and swelling. The shoulder may appear squared off rather than rounded. First-time
dislocations carry a risk of recurrence, particularly in younger individuals.
7. Achilles Tendon Injuries
What it is: Strain, inflammation
(tendinopathy), or rupture of the Achilles
tendon, the thick band of tissue connecting the calf muscles to the heel bone. It is the
largest tendon in the body.
Achilles tendon rupture rates range from 7 to 40 per
100,000 people per year globally, with incidence rising across all studied countries over
the past few decades.
Cause: Repetitive overuse from running or jumping, sudden increases in training
intensity, or an abrupt explosive movement such as a sprint start.
Frequently seen in: Running, basketball, badminton, football, and tennis.
Common symptoms: Tendinopathy causes pain and stiffness at the back of the heel,
often worse in the morning or after activity. A rupture typically produces a sudden snap or pop,
followed by sharp pain and difficulty pushing off the foot.
8. Shin Splints
What it is: Shin splints,
known medically as medial tibial stress syndrome, refers to pain along the inner edge of the
shinbone (tibia) caused by stress on the bone and surrounding tissues.
Studies estimate that shin splints affect between 5 and 35 per cent of
runners, with higher rates among beginners and military personnel.

Cause: Repetitive impact on hard surfaces, sudden increases in training volume or
intensity, flat feet, and worn-out footwear. The muscles, tendons, and bone tissue around the tibia
become overloaded.
Frequently seen in: Running, dancing, military training, and court sports such as
basketball and tennis.
Common symptoms: A dull, aching pain along the front or inner part of the lower leg
during and after exercise. The area may be tender to touch. Pain typically eases with rest but
returns with activity.
9. Runner's Knee (Patellofemoral Pain Syndrome)
What it is: Patellofemoral pain
syndrome, commonly called runner's knee, is pain around or behind the kneecap caused by
irritation of the cartilage on its underside or poor tracking of the kneecap within its groove.
Patellofemoral pain has an annual prevalence of roughly 23 per cent in the general population and
accounts for up to 25 per cent of all running-related injuries.
Cause: Overuse from repetitive bending
of the knee, muscle imbalances (particularly weak quadriceps or hip muscles), flat feet, and
activities that place repeated stress on the knee joint.
Frequently seen in: Running, cycling, hiking, and sports involving frequent
squatting or jumping.
Common symptoms: Aching pain around the kneecap that worsens when climbing stairs,
squatting, sitting for long periods, or running downhill. You may also notice a grinding or clicking
sensation when bending the knee.
10. Tennis Elbow (Lateral Epicondylitis)
What it is: Tennis elbow is
inflammation or micro-tearing of the tendons that attach to the bony bump on the outer side of the
elbow. These tendons connect the forearm muscles used to extend the wrist and fingers.
Tennis elbow affects an estimated 1 to 3 per cent
of the adult population globally, with peak incidence between the ages of 35 and 55.
Cause: Repetitive gripping, twisting, or wrist extension movements that overload
the forearm tendons. Despite its name, most cases are not caused by tennis.
Frequently seen in: Racquet sports, golf, weight training, and occupations or
hobbies involving repetitive hand and wrist movements.
Common symptoms: Pain and tenderness on the outer elbow that may radiate down the
forearm. Gripping objects, turning a door handle, or shaking hands can worsen the pain. Symptoms
often develop gradually over weeks.
How Are Sports Injuries Diagnosed?
Diagnosis of sports injuries typically involves a combination of clinical assessment and imaging to identify the affected structure and the severity of damage.
- Clinical history – Understanding how the injury occurred, the symptoms experienced, and any previous injuries helps narrow down the likely diagnosis
- Physical examination – Testing the affected area for swelling, tenderness, range of motion, strength, and joint stability. Specific clinical tests, such as the Lachman test for ACL injuries or the anterior drawer test for ankle sprains, can help identify which structure is involved
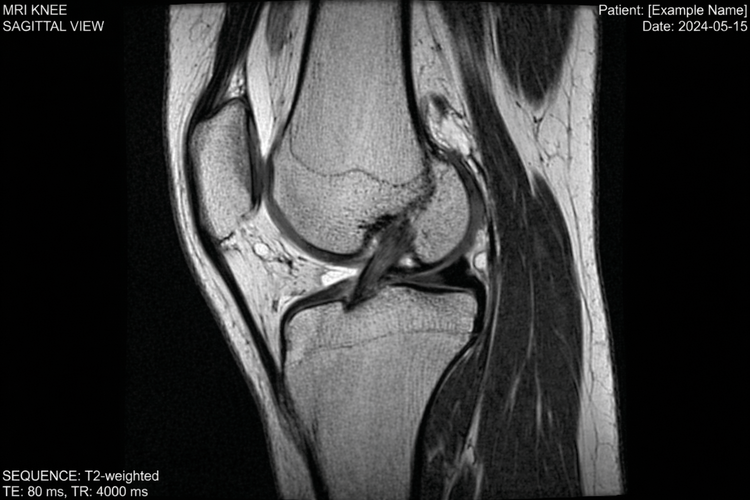
- Imaging – X-rays are used to check for fractures, while MRI provides detailed views of soft tissues such as ligaments, tendons, and cartilage. Ultrasound may also be used for tendon and muscle injuries
The type and extent of imaging depends on the clinical findings. Not every injury requires advanced imaging, and the clinical examination often provides enough information to guide initial treatment.
Treatment Options for Sports Injuries
Treatment depends on the type, severity, and location of the injury, as well as the
individual's activity goals and overall health.
Non-surgical treatment is typically prioritised first, with surgery considered when conservative
approaches are insufficient or when the injury requires structural repair.
| Treatment | Description | Commonly Used For |
|---|---|---|
| Non-Surgical Treatments | ||
| Rest, Ice, Compression, Elevation (RICE) | Relieves pain, limits swelling, and protects the injured area in the early phase. May involve temporary use of crutches, bracing, or splints to offload the joint. | Most sports injuries, especially in the acute phase |
| Anti-inflammatory medication | Oral or topical drugs such as NSAIDs that reduce inflammation and provide short-term pain relief. | Most sports injuries, used cautiously with ligament injuries |
| Physiotherapy | A structured rehabilitation programme to restore strength, flexibility, movement patterns, and joint stability through targeted exercises and manual techniques. | Used for most sports injuries and tailored to specific recovery stages |
| Bracing or taping | External supports that limit excessive movement and protect healing tissues during activity and return to sport. | Ligament sprains, joint instability, and post-surgical rehabilitation |
| Injection therapies (cortisone, PRP, hyaluronic acid) | Targeted injections to reduce inflammation, relieve pain, or support tissue healing. Cortisone calms inflammation, PRP aids tissue repair, and hyaluronic acid improves joint lubrication. | Persistent pain, tendon injuries, and chronic joint irritation |
| Shockwave therapy | A non-invasive procedure that delivers sound waves to injured tissue to promote healing. | Chronic tendon pain such as Achilles tendinopathy and tennis elbow |
| Surgical Treatments | ||
| Ankle ligament reconstruction | Surgical repair or reconstruction of damaged ankle ligaments to restore joint stability. | Chronic ankle instability that has not responded to rehabilitation |
| ACL reconstruction | Replacement of the damaged ligament with a graft from the hamstring, patellar tendon, or a donor using an arthroscope. | Complete ACL tears in active individuals returning to pivoting sports |
| Meniscus repair or trimming | Arthroscopic surgery to stitch the torn meniscus or remove the damaged portion to relieve symptoms. | Meniscus tears causing persistent locking, catching, or pain |
| Shoulder stabilisation (Bankart repair) | Reattachment of the torn labrum and tightening of the shoulder capsule to prevent recurrent dislocation. | Recurrent shoulder dislocations, particularly in younger athletes |
When to See a Doctor for a Sports Injury
Many minor sports injuries, such as mild strains and bruises, improve with rest, ice, and over-the-counter pain relief. However, you should seek medical attention if you experience any of the following:
- Inability to bear weight or use the affected limb
- Significant swelling, bruising, or deformity around a joint
- A popping or snapping sensation at the time of injury
- Joint instability, locking, or giving way
- Numbness or tingling in the affected area
- Severe pain that does not improve within a few days
- Symptoms that keep returning with activity despite rest
Early assessment is particularly important for suspected ligament tears, fractures, and dislocations, as delayed treatment can lead to complications such as chronic instability, cartilage damage, or prolonged recovery.
Sports injuries can affect anyone, whether you play competitively or exercise recreationally. A thorough clinical assessment helps identify the specific structures involved, so treatment can be tailored to the injury and your activity goals.
Find a Sports Doctor in Singapore
Apex Novena
Why Do Patients Choose Apex Sports Clinic?
Sports Doctor in Singapore: Personalised & Affordable Care
Progressive Treatment Philosophy
We prioritise personalised, non-invasive solutions, progressing to specialised treatments, including surgery, only when needed for more effective and targeted care.
Keyhole Surgery Expertise
We specialise in advanced arthroscopic keyhole surgery to treat sports injuries with precision and minimal tissue disruption, supporting faster recovery and restored joint function.
Specialist in Sports Orthopaedics & Injury Management
We combine expert injury management with a proactive approach to maintaining your body's strength and function, so you can recover fully and perform at your peak.
Patient Journey
1 . Schedule Your Appointment

2 . Expert Diagnosis & Consultation

3 . Customised Treatment Plan

Schedule an Appointment

Our Insurance Partners








Frequently Asked Questions (FAQs)
The five most common sports injuries are ankle sprains, ACL tears, meniscus tears, hamstring strains, and runner's knee (patellofemoral pain syndrome). Ankle sprains alone account for an estimated 20 to 40 per cent of all athletic injuries, making them the single most frequent sports injury worldwide. These injuries affect a wide range of physically active individuals, from recreational exercisers to competitive athletes.
Signs that a sports injury may be serious include an inability to bear weight, significant swelling or deformity around a joint, a popping or snapping sensation at the time of injury, and joint instability or locking. Numbness, tingling, or pain that does not improve within a few days also warrant attention. If you experience any of these symptoms, you should seek prompt medical evaluation to prevent further complications.
Not all sports injuries require medical attention. Minor strains and bruises often improve with rest, ice, and over-the-counter pain relief. However, you should seek prompt medical attention if you experience severe pain, significant swelling, joint instability, or difficulty using the affected limb. Early assessment is particularly important for suspected ligament tears, fractures, and dislocations, as delayed treatment can lead to complications such as chronic instability or prolonged recovery.
Recovery time depends on the type and severity of the injury. Mild strains and sprains may resolve within a few weeks with rest and rehabilitation, while ligament tears or fractures can take several months. Surgical injuries such as ACL reconstruction typically require 6 to 12 months before return to sport. Factors such as age, overall health, adherence to rehabilitation, and the demands of the sport also influence recovery timelines.
A sprain is an injury to a ligament, the tissue that connects bones at a joint, caused by stretching or tearing. A strain is an injury to a muscle or tendon, the tissue that connects muscle to bone. Sprains commonly affect the ankle and knee, while strains often occur in the hamstring or calf. Both injuries range from mild stretches to complete tears and are treated based on their severity and location.
You should return to sport only when the injured area has regained adequate strength, flexibility, and stability, and you can perform sport-specific movements without pain. Returning too early increases the risk of re-injury and may lead to longer-term complications. Recovery timelines vary depending on the injury, ranging from weeks for minor strains to several months based on the treatment required. It is advisable to consult your doctor, specialist, or physiotherapist before resuming full activity.
No, most sports injuries do not require surgery. Non-surgical treatments such as rest, physiotherapy, bracing, and injection therapies are typically prioritised first and are sufficient for many conditions. Surgery is generally considered when conservative approaches have not relieved symptoms or when the injury involves structural damage that cannot heal adequately on its own, such as a complete ACL tear in an active individual or recurrent shoulder dislocations.
The most common knee injury in sports is patellofemoral pain syndrome, also known as runner's knee, which accounts for a significant proportion of knee-related complaints in active individuals. ACL tears and meniscus tears are also highly prevalent, particularly in sports involving pivoting, jumping, and sudden direction changes such as football, basketball, and netball. The specific injury risk depends on the sport, the individual's age, and the type of movements involved.
Contact sports such as football, rugby, and basketball consistently report the highest overall injury rates due to the combination of physical collisions, rapid direction changes, and high-speed movements. Running-based sports also carry significant injury risk, particularly for overuse conditions affecting the knee, shin, and Achilles tendon. However, injury rates vary depending on how they are measured, whether by total number, exposure time, or severity, so direct comparisons across sports should be interpreted with caution.
Pain is subjective and varies between individuals, but injuries commonly reported as among the most painful include shoulder dislocations, Achilles tendon ruptures, ACL tears, and fractures. Shoulder dislocations often cause intense immediate pain with visible deformity, while Achilles ruptures produce a sudden sharp pain that can make walking difficult. The level of pain experienced depends on the severity of the injury, the structures involved, and individual pain tolerance.
There is no single sport that is universally the easiest to get injured in, as injury risk depends on factors such as the level of physical contact, training intensity, playing surface, and individual conditioning. However, contact sports like rugby and football tend to have higher overall injury rates, while running and court sports carry a higher risk of overuse injuries. Beginners in any sport face elevated risk due to insufficient conditioning and unfamiliar movement patterns.
The most severe sports injuries are typically those that require surgery and involve prolonged rehabilitation, such as complete ACL tears, Achilles tendon ruptures, shoulder dislocations with structural damage, and complex fractures. These injuries can sideline individuals for 6 to 12 months or longer and may carry a risk of long-term complications such as chronic instability, re-injury, or early joint degeneration. Severity depends on the structures damaged and the demands of the individual's sport.
Many individuals recover well after ACL reconstruction and return to sport, but outcomes vary. A significant proportion of athletes return to their previous level of sport following surgery and rehabilitation. However, factors such as age, re-injury risk, adherence to rehabilitation, and the presence of additional damage to the meniscus or cartilage influence long-term outcomes. If you have sustained or suspect an ACL tear, it is best to consult your specialist on expectations for recovery.
Female athletes are at a notably higher risk of ACL tears than males, particularly in comparable sports such as football and basketball. Contributing factors include anatomical differences such as a wider pelvis and smaller intercondylar notch, hormonal influences on ligament laxity, and movement patterns such as the knees turning inward during landing. Injury prevention programmes focusing on landing mechanics and strengthening exercises have been shown to help reduce this risk.

