Radiofrequency Ablation in Singapore
Information reviewed by: Dr Foo Gen Lin | Last updated:
Chronic joint or spinal pain limiting your daily activities? Dr Foo provides radiofrequency ablation as a non-surgical option to help manage persistent pain to achieve longer lasting relief.
MBBS (University of London) | MMed (Ortho) | FRCSEd (Ortho) | FAMS (Ortho)

What Is Radiofrequency Ablation?
Radiofrequency ablation (RFA) is a minimally invasive, image-guided procedure that
uses heat energy to interrupt the nerves responsible for transmitting chronic pain
signals to the brain.
During treatment, a specialised needle is positioned near the target nerve under X-ray or
ultrasound guidance, then delivers controlled radiofrequency energy that heats the nerve
tissue to form a small lesion. The result is a reduction or blockage of pain signals, with
relief that can last several months to over a year.
RFA is commonly considered for chronic lower back, neck, or knee pain when
conservative
treatments such as physiotherapy, medication, and injections have not provided
lasting relief, and as a non-surgical option to delay or avoid surgery.
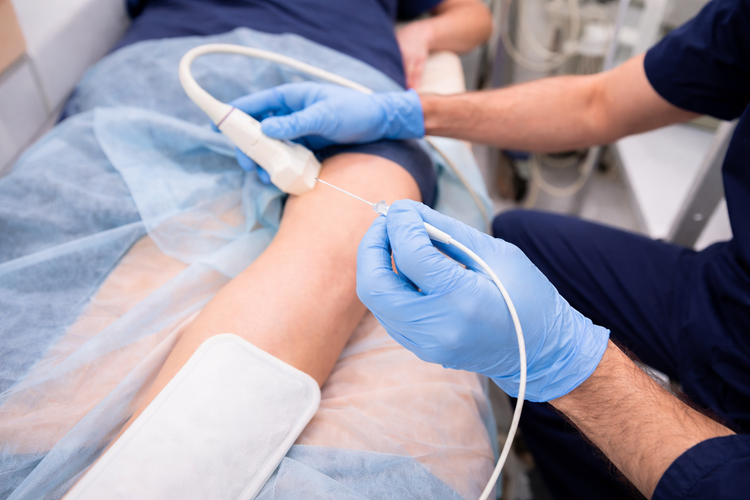
How Does Radiofrequency Ablation Work?
Radiofrequency ablation works by delivering controlled thermal
energy through a thin, insulated needle electrode to specific sensory nerves that carry pain
signals. The heat creates a small, precise lesion on the nerve, which disrupts its ability
to transmit pain signals to the brain.
Because the procedure targets sensory rather than motor nerves, it does not typically affect muscle
strength or movement in the treated area.
Before undergoing RFA for the first time, your doctor will usually perform a diagnostic nerve block.
This involves injecting a small amount of local anaesthetic near the suspected nerve to temporarily
numb it and confirm that it is the source of pain.
Types of Radiofrequency Ablation

There are two main types of radiofrequency ablation used, each suited to different conditions and treatment goals.
Conventional (Thermal) Radiofrequency Ablation
Conventional RFA applies continuous
heat at temperatures of 60°C to 90°C to create a thermal lesion on the targeted
nerve.
This approach is commonly used for chronic pain originating from the facet joints of the
spine, sacroiliac joint, and knee. It typically provides longer-lasting pain relief.
Pulsed Radiofrequency Ablation
Pulsed RFA delivers short bursts of radiofrequency
energy at lower temperatures, usually below 42°C. Instead of destroying the nerve, it
alters how the nerve sends pain signals.
This approach may be considered for conditions involving mixed sensory and motor nerves, where
preserving nerve integrity is important. Pulsed RFA is commonly applied for peripheral nerve pain
and certain joint conditions.
Conditions Treated with Radiofrequency Ablation
Radiofrequency ablation is used to manage a range of chronic pain conditions, particularly those affecting the spine, joints, and surrounding tissues.
Facet Joint Pain
Facet joint
pain is chronic neck or back pain arising from the small joints that connect each
vertebra. These joints can become inflamed or damaged due to ageing, repetitive stress,
or spinal degeneration.
How RFA works: Targets the medial branch nerves, which are small sensory nerves
that carry pain signals from the facet joints, reducing pain transmission from these joints. It is
one of the most commonly performed and well-studied uses of this procedure.
Sacroiliac Joint Pain
Sacroiliac joint pain causes persistent discomfort in
the lower back and buttock region due to dysfunction of the joint that connects the
base of the spine to the pelvis. This pain is often aggravated by prolonged standing, climbing
stairs, or transitioning between sitting and standing.
How RFA works: Targets the lateral branch nerves that supply the sacroiliac joint,
helping reduce chronic pain when conservative treatments have not provided sufficient relief.
Knee Osteoarthritis
Knee osteoarthritis
is a degenerative condition where cartilage in the knee joint gradually wears down, leading
to chronic pain and stiffness.
How RFA works: Targets the genicular nerves, which are sensory nerves
surrounding the knee joint, to reduce pain signalling. This approach is increasingly used
for individuals who may not be suitable candidates for surgery or who wish to delay knee replacement.
Hip Joint Pain
Hip joint pain often results from osteoarthritis or other degenerative changes that
cause persistent discomfort in the hip and groin area.
How RFA works: Targets the sensory nerves supplying the hip joint to reduce pain
transmission, particularly when physiotherapy or injections have not provided adequate relief.
Chronic Neck Pain
Chronic neck pain frequently originates from degenerative changes or wear in the facet
joints of the cervical spine, and is commonly associated with age-related joint
deterioration or whiplash injuries.
How RFA works: Targets the medial branch nerves in the cervical spine, which are
small sensory nerves that carry pain signals from the affected facet joints. This follows the same
principle as facet joint ablation in the lower back.
Peripheral Nerve Pain
Peripheral nerve pain involves localised discomfort caused by
irritation or damage to specific nerves outside the brain and spinal cord.
How RFA works: Alters how the affected nerve transmits pain signals, helping to
reduce discomfort. Pulsed radiofrequency is more commonly used in these cases, as it does not
destroy the nerve but instead changes how it functions to ease symptoms.
What to Expect During a Radiofrequency Ablation Procedure
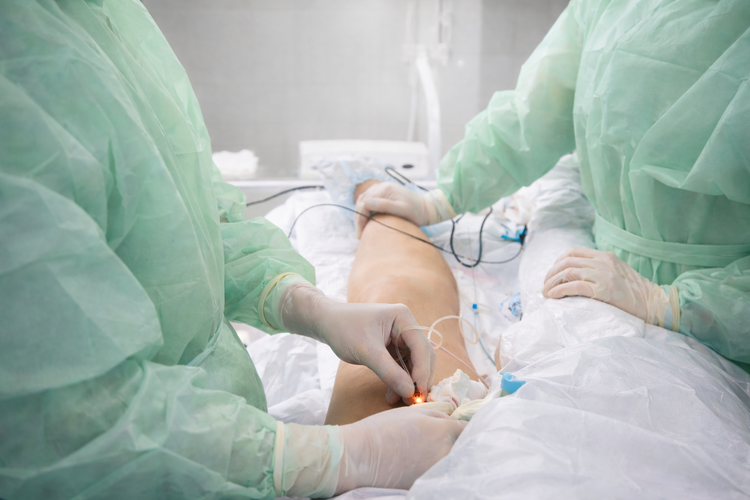
Radiofrequency ablation is typically performed as an outpatient procedure under
local anaesthesia, meaning you can return home on the same day.
The process usually involves the following steps:
- Imaging and needle placement – Fluoroscopy (live X-ray) or ultrasound guides a thin needle to the targeted nerve.
- Nerve confirmation – Brief electrical stimulation helps confirm that the needle is positioned near the correct sensory nerve.
- Ablation – Radiofrequency energy is delivered to create a controlled lesion on the nerve, reducing its ability to transmit pain signals.
The treatment typically takes between 30 and 90 minutes, depending on the number of nerves involved. Sedation may be offered where appropriate.
Recovery After Radiofrequency Ablation
Most individuals resume light activities within 24 to 48 hours, with full pain
relief typically developing over 2 to 4 weeks as the treated nerve responds to
the lesion. You may experience mild soreness or swelling at the treatment site for the first one
to two weeks.
Physiotherapy may be recommended to maintain mobility, and a follow-up appointment is typically
scheduled to assess your response to treatment.
Always follow your orthopaedic specialist's post-procedure instructions to support proper
recovery and reduce the risk of complications.
How Long Do the Effects of Radiofrequency Ablation Last?
The effects of radiofrequency ablation typically last between 6 and 12 months,
although the duration varies depending on the condition treated and individual response.
RFA works by disrupting pain-transmitting sensory nerves, but these nerves can gradually
regenerate over time. As the nerve heals, pain signals may slowly return. If you previously
experienced meaningful relief, the procedure may be repeated after reassessment.
The diagnostic nerve block performed before RFA can help predict whether the procedure is likely
to provide longer-lasting pain relief.
Potential Side Effects of Radiofrequency Ablation
Radiofrequency ablation is a minimally invasive procedure, but as with any medical intervention, it carries potential side effects. Most are mild and temporary:
- Soreness at the treatment site
- Mild swelling or bruising
- Temporary pain flare in the first few days
- Numbness or tingling near the treated area
Less common side effects include:
- Infection at the needle insertion site
- Allergic reaction to the local anaesthetic or other medications used during the procedure
- Partial or insufficient pain relief, especially if there is pain from multiple sources or if the treated nerve is not the sole cause of symptoms
- Inadvertent irritation or injury to a nearby nerve, which can lead to prolonged numbness, weakness, or altered sensation
Disclaimer: This is not a complete list of all possible side effects. You should discuss the potential risks and benefits of RFA with your specialist to determine whether it is appropriate for your condition.
Radiofrequency Ablation vs Other Pain Management Options
Radiofrequency ablation differs from other pain treatments by directly interrupting
pain-transmitting nerves. It typically provides longer-lasting relief than injections
while remaining less invasive than surgery.
Here is how it compares with other treatment options:
| Treatment | How It Works | Duration of Relief | Considerations |
|---|---|---|---|
| Radiofrequency Ablation | Disrupts pain-transmitting nerves using heat | 6–12+ months | Minimally invasive and may be repeated if pain returns |
| Oral Medication (e.g. NSAIDs) | Reduces pain and inflammation through systemic medication | Hours to days | Provides temporary relief and may cause side effects with long-term use |
| Corticosteroid Injection | Reduces inflammation at the joint or around a nerve | Weeks to months | Relief is temporary and repeated use may weaken surrounding tissues |
| Epidural Steroid Injection | Reduces inflammation around irritated spinal nerve roots | Weeks to months | Commonly used for radicular pain; relief may be temporary |
| Shockwave Therapy | Uses acoustic waves to stimulate healing and improve blood flow | Varies and often requires multiple sessions | Non-invasive and commonly used for tendon-related pain |
| Platelet-Rich Plasma (PRP) Injection | Uses concentrated platelets from your blood to support tissue healing | Varies and develops gradually | Aims to improve underlying tissue health, with pain relief developing gradually as healing occurs |
| Physiotherapy | Strengthens muscles and improves joint stability and movement | Ongoing with continued exercise | Non-invasive and often used alongside other treatments |
| Surgery (e.g. Joint Replacement) | Repairs or replaces damaged joint structures | Long-term | Usually considered when non-surgical treatments have not provided adequate relief |
How Much Does Radiofrequency Ablation Cost in Singapore?
At Apex Sports Clinic, we offer radiofrequency ablation as one of several non-surgical treatment options for chronic pain conditions, with the prices as follows:
| Procedure | Estimated Cost (SGD)* |
|---|---|
| Initial Consultation | From $200 |
| Follow-Up Consultation | From $150 |
| Second Opinion Consultation | From $200 |
| Radiofrequency Ablation (RFA) | From $3,000 |
MediSave may be used for selected approved procedures, including radiofrequency ablation, subject to your diagnosis and eligibility under Ministry of Health guidelines. For more information on MediSave claims and eligibility, please contact our clinic for assistance.
Is Radiofrequency Ablation Right for You?
Radiofrequency ablation may be suitable if you:
- Experience chronic joint or spinal pain lasting more than 3 months
- Have not responded to conservative measures such as physiotherapy, medication, or injections
- Wish to reduce reliance on long-term pain medication
- Have been advised that surgery may not be appropriate at this time
RFA may not be recommended for individuals with active infections at the treatment site, certain
bleeding disorders, or those who are pregnant.
A thorough evaluation of your condition and medical history is necessary to determine if the
procedure is appropriate.
Radiofrequency ablation can help manage chronic pain by targeting the specific nerves responsible for transmitting discomfort. When paired with a thorough assessment and a confirmed diagnostic nerve block, it offers a meaningful non-surgical option for pain relief.
Find an Orthopaedic Specialist in Singapore
Apex Novena
Why Do Patients Choose Apex Sports Clinic?
Sports Doctor in Singapore: Personalised & Affordable Care
Progressive Treatment Philosophy
We prioritise personalised, non-invasive solutions, progressing to specialised treatments, including surgery, only when needed for more effective and targeted care.
Keyhole Surgery Expertise
We specialise in advanced arthroscopic keyhole surgery to treat sports injuries with precision and minimal tissue disruption, supporting faster recovery and restored joint function.
Specialist in Sports Orthopaedics & Injury Management
We combine expert injury management with a proactive approach to maintaining your body's strength and function, so you can recover fully and perform at your peak.
Patient Journey
1 . Schedule Your Appointment

2 . Expert Diagnosis & Consultation

3 . Customised Treatment Plan

Schedule an Appointment

Our Insurance Partners








Frequently Asked Questions (FAQs)
The main downsides of radiofrequency ablation include temporary soreness, swelling, bruising, numbness, or a short-term pain flare after the procedure. Less common risks include infection, allergic reaction, insufficient pain relief, or irritation of a nearby nerve that may cause prolonged numbness or weakness. Results vary between individuals, and symptoms can return as nerves regenerate. Nevertheless, many people experience meaningful improvement when the pain source is accurately identified.
Radiofrequency ablation is generally not recommended for individuals with active infection at the treatment site, certain bleeding disorders, uncontrolled medical conditions, or during pregnancy. It may also be unsuitable if the pain does not originate from the targeted nerve. A thorough assessment of the diagnosis, imaging findings, and overall health is required to determine whether the procedure is appropriate.
If radiofrequency ablation does not provide sufficient relief, the next step depends on the underlying cause of pain and the treatments already tried. Options may include reassessment of the diagnosis, physiotherapy, alternative injections, regenerative treatments such as PRP, or surgical consideration where appropriate. It is best to discuss your ongoing symptoms with your orthopaedic specialist to determine the most suitable next step.
Radiofrequency ablation is not inherently better than surgery; it serves a different role in pain management. RFA is minimally invasive and aims to reduce pain by interrupting nerve signals, while surgery addresses structural problems such as severe joint degeneration or instability. For some individuals, RFA may help delay or avoid surgery, whereas others may ultimately require operative treatment. It is advisable to consult an orthopaedic specialist who can assess your condition and advise on an appropriate treatment plan.
Radiofrequency ablation is generally considered for individuals with chronic joint or spinal pain lasting more than three months that has not improved with physiotherapy, medication, or injections. It is typically offered when assessment suggests the pain originates from specific sensory nerves and confirmation is obtained as part of the RFA evaluation process. It is best to consult an orthopaedic specialist to determine whether this procedure is suitable for you.
Recovery after radiofrequency ablation is generally short, with most individuals resuming light activities within 24 to 48 hours. Mild soreness or swelling can occur for one to two weeks, and pain relief often develops gradually over two to four weeks. Strenuous activity is usually limited for the first few days. Your orthopaedic specialist will provide specific post-procedure guidance based on your condition.
Most radiofrequency ablation procedures are performed under local anaesthesia, so you remain awake but the treated area is numbed. Some individuals may receive light sedation to improve comfort, depending on the location treated and personal preference. You may feel pressure or brief tingling during nerve testing, but significant pain is uncommon. Your orthopaedic specialist will explain the anaesthesia plan before the procedure.
Radiofrequency ablation is typically repeated only if pain returns after an initial period of relief, which often lasts six to twelve months. The treated nerve can gradually regenerate, allowing symptoms to recur over time. Repeat procedures may be considered if the first treatment provided meaningful benefit and reassessment confirms the same pain source. It is best to follow up with your orthopaedic specialist to determine whether another session is appropriate.
When radiofrequency ablation wears off, the treated nerve may regenerate and begin transmitting pain signals again, leading to a gradual return of symptoms. The timing varies between individuals and conditions. If pain recurs, your orthopaedic doctor may reassess the diagnosis and discuss options such as repeat ablation, injections, physiotherapy, or other treatments depending on your overall condition.
After radiofrequency ablation, you may be advised to avoid strenuous exercise, heavy lifting, and high-impact activities for the first few days to allow the treated area to settle. Most individuals resume light activities within 24 to 48 hours, although mild soreness or swelling can last one to two weeks. Always follow your orthopaedic specialist's post-procedure guidance to support proper recovery.

